We Ask the Experts: What You Should Know About Ovarian Cancer
BY CAMILLE PLATT


Gynecologist,
CHI Memorial
Women’s Health Associates
According to the National Ovarian Cancer Coalition, ovarian cancer is the fifth leading cause of cancer-related deaths in women ages 35-74. Dr. Michael Pippin, a gynecologist with CHI Memorial Women’s Health Associates, explains, “Each year we’ll see approximately 22,000 new cases of ovarian cancer diagnosed and about 14,000 ovarian cancer-related deaths. That makes ovarian cancer the deadliest female pelvic cancer.”
In its early stages, ovarian cancer is often without symptoms, which means by the time you notice something is wrong, it’s likely had a chance to spread. If diagnosed and treated early, the five-year survival rate is 90%. Unfortunately, this only accounts for about 1 in 5 patients.
Dr. Christopher J. Radpour, an OB-GYN with Galen Obstetrics & Gynecology, explains, “Ovarian cancer is cancer that affects one or both ovaries, either on the surface – this is called ‘epithelial’ ovarian cancer and accounts for 90% of diagnoses – or in the deeper tissues of the ovary, which accounts for 10% of ovarian cancers.” One in 78 women will face an ovarian cancer diagnosis in her lifetime.
Detection Difficulty


OB-GYN, Galen Obstetrics & Gynecology
The symptoms of an early stage ovarian cancer are vague. As they intensify, it’s also easy to mistake them for other diseases and disorders. You may have bloating or abdominal pain, back pain, changes in your menstrual cycle, or you may notice the need to urinate more frequently than usual. You may also experience a sudden change in weight, unexpected fullness when eating, fatigue, or pain during intercourse. Unfortunately, if ovarian cancer remains undetected until stage 3 or higher, the survival rate can drop as low as 28%.
To increase your chances of detecting ovarian cancer early, it’s imperative you don’t ignore symptoms, even if you’re hopeful you will find relief with a change in diet, exercise, or rest. If you experience any of the symptoms above and they persist, speak to your doctor about your concerns.
Dr. Radpour agrees. “Routine yearly gynecological exams are a good way to ensure that your uterus, fallopian tubes, and ovaries are normal and stable in size. If you have any combination of ovarian cancer symptoms, especially lasting more than two to three weeks, make an appointment with your gynecologist.
A pelvic exam can check for ‘fullness’ in the area where the ovaries lie, and a pelvic ultrasound can give us further information.” A CA-125 blood test can reveal high levels of a protein that can suggest an ovarian cancer diagnosis. However, other non-cancerous conditions can also lead to elevated levels of the CA-125 protein, so this test is generally only recommended for women at high risk for ovarian cancer.
YOUR YEARLY CHECKUP
Your yearly checkup is the perfect opportunity to bring up any concerns you might have about your health. “This is the time you want to mention everything that’s been on your mind,” says Dr. Pippin. “You don’t want to say to yourself, ‘I’m being overdramatic,’ or, ‘I don’t want to bother the doctor with something insignificant.’ Having a high index of suspicion will help your doctor diagnose problems early.”

So, Who’s at Risk?
Ovarian cancer is most common in women ages 50-60. Your risk of a diagnosis goes up with age, with infertility, and if you experienced a rather early first menses or rather late menopause. “Family history is also an important risk factor,” explains Dr. Shae Connor, a gynecologic oncologist with Erlanger Gynecologic Oncology. “Several genetic mutations have been identified in recent years that increase a woman’s lifetime risk of ovarian cancer. BRCA1 and BRCA2 mutations are the most common cause of hereditary ovarian cancer, but several other genes have been identified as well. Any woman with a strong family history of breast or ovarian cancers should talk to her doctor about genetic testing.”
Of course, the reality is that some women with multiple risk factors will never get ovarian cancer, while others who never identified a reason for early detection do.
DID YOU KNOW?
The risk of ovarian cancer increases with the number of times a woman ovulates in her lifetime. Dr. Radpour explains, “A woman who starts her period later in life, for example at age 12 or 13 rather than at age 8 or 9, and/or who goes through menopause earlier, for example at age 50 as opposed to age 55, will ovulate fewer times in her lifetime. This puts her at a lower risk of epithelial ovarian cancer.” Similarly, he says, “A woman who takes birth control pills, experiences one or more pregnancies, and/or who breastfeeds for much of her reproductive life will have a lower risk.”
Treatment Options


Gynecologic Oncologist,
Erlanger Gynecologic Oncology
After a diagnosis, decisions about treatment will depend on the stage of your ovarian cancer and your doctor’s recommendations. “Every woman with ovarian cancer should be evaluated by a gynecologic oncologist,” shares Dr. Connor. “Gynecologic oncologists are experts in both the surgical and medical management of ovarian cancer, and studies have shown that women live longer and have better outcomes when they receive treatment from a gynecologic oncologist.”
An initial surgery will remove all visible signs of cancer and, depending on the severity, may result in the removal of one or both ovaries, fallopian tubes, and possibly the uterus. This surgery will help your physician collaborate with a pathologist to stage the cancer.
“Stage 1 means the cancer is still confined to the ovary,” explains Dr. Pippin. “Stage 2 means it’s spread to the pelvis, stage 3 means it’s spread throughout the abdominal cavity, and stage 4 means it’s spread beyond the abdomen. Most ovarian cancer is diagnosed at stage 3.”
If your doctor recommends chemotherapy, know that the goal here is to both stop cancer cells from growing and destroy the cancer cells completely. This can be helpful in shrinking tumors.
Next, a less invasive surgery will allow your oncologist to make sure your body is responding well to chemotherapy.
In addition to standard treatment, some women choose to pursue complementary therapies to lessen the side effects of cancer. Different from alternative medicine, (which is used in place of standard treatment), complementary therapies are added to standard treatment to relieve nausea, stress, pain, and fatigue and include aromatherapy, massage, yoga, meditation, and acupuncture. Your health care team can help direct you toward therapies that best fit for your preferences and lifestyle.
“Every woman with ovarian cancer should be evaluated by a gynecologic oncologist. Gynecologic oncologists are experts in both the surgical and medical management of ovarian cancer, and studies have shown that women live longer and have better outcomes when they receive treatment from a gynecologic oncologist.”
–Dr. Shae Connor
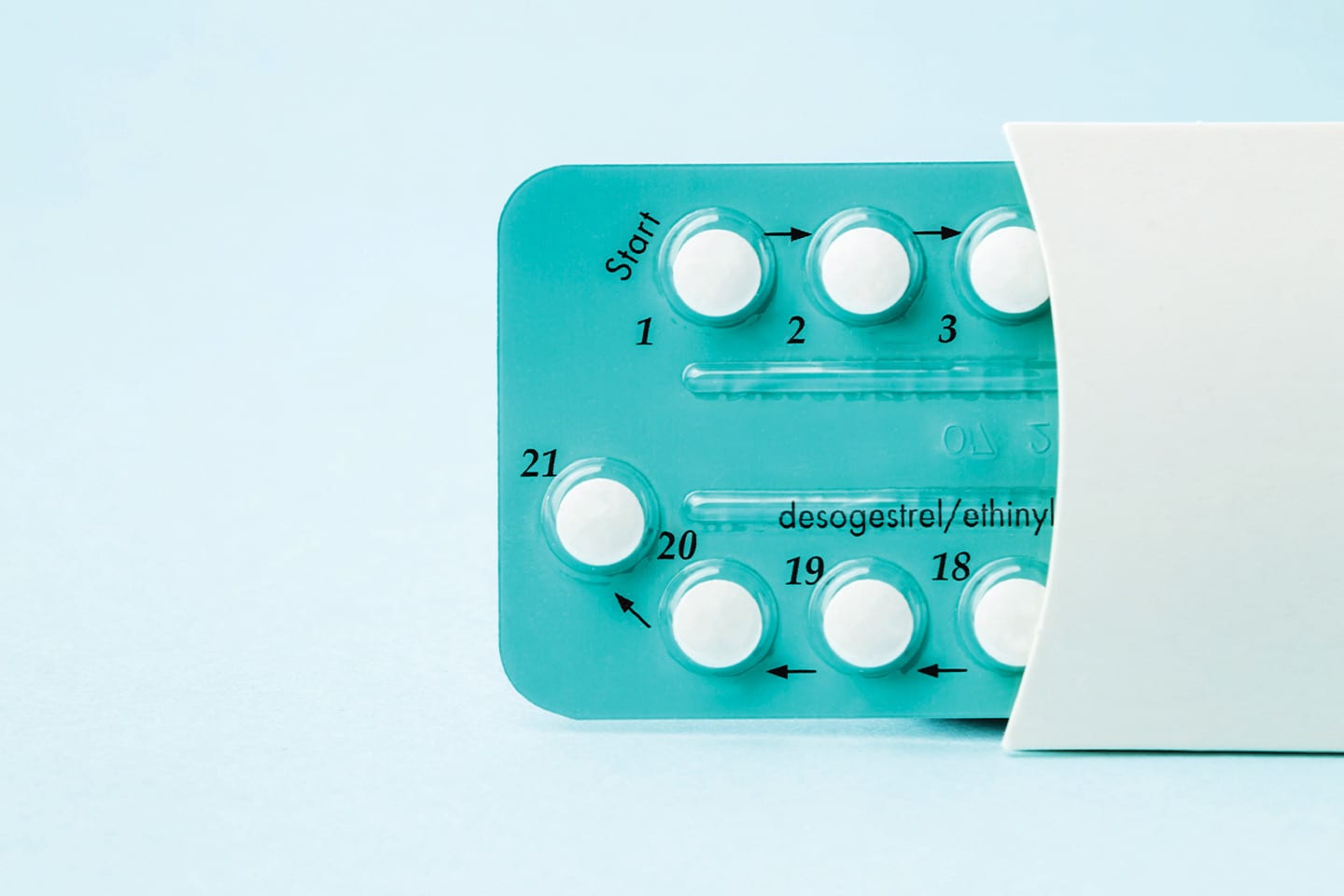

According to the American Cancer Society, women who use birth control pills for five or more years lower their chances of developing ovarian cancer by 50%. However, birth control pills may increase your risk of other health problems, so be sure to review the risks and benefits with your doctor before choosing a contraception method.
Can It Be Prevented?
There is no way to eliminate your risk of ovarian cancer, but you can proactively reduce your risk by paying attention to the factors under your control. In addition to maintaining a healthy weight, childbirth, specifically carrying a pregnancy to term before age 35, and choosing to breastfeed can lower your risk. A study published in The American Journal of Clinical Nutrition found that extended breastfeeding – 13 months or longer – reduced a woman’s chances of developing an ovarian tumor by 63%. Breastfeeding delays ovulation, and the more times a woman ovulates, the greater the chance of cell mutation.
Tubal ligation and hysterectomy also lower a woman’s risk for ovarian cancer, but physicians agree these procedures should never be done for ovarian cancer prevention alone. Research has also shown that for many women who carry the BRCA genetic mutation and are still premenopausal, removal of the ovaries reduces the risk of ovarian cancer by 85-95% and reduces the risk of breast cancer by at least 50%.
Women who consistently track and monitor changes in their health, and who talk openly about women’s health issues with their peers and their physicians, are empowered to catch a gynecologic cancer early for fast, effective treatment. “Ovarian cancer is not a death sentence,” says Dr. Connor. “With modern surgical and medical management, many women live with ovarian cancer for an extended period of time. Even when a cure is not possible, treatment to extend both the quantity and quality of life is an achievable goal.” HS

