Here’s the scenario: You walk out of your warm and cozy house to go to the mailbox one winter day, and before you get there, you have two or three fingers suddenly white and numb – what happened? It may be Raynaud’s, a syndrome that causes vasospasms, or spasms in your blood vessels, that can stop the flow of blood to your fingers and toes, and sometimes even your ears or nose. Find out what causes the attacks, and what you can do to lessen them.
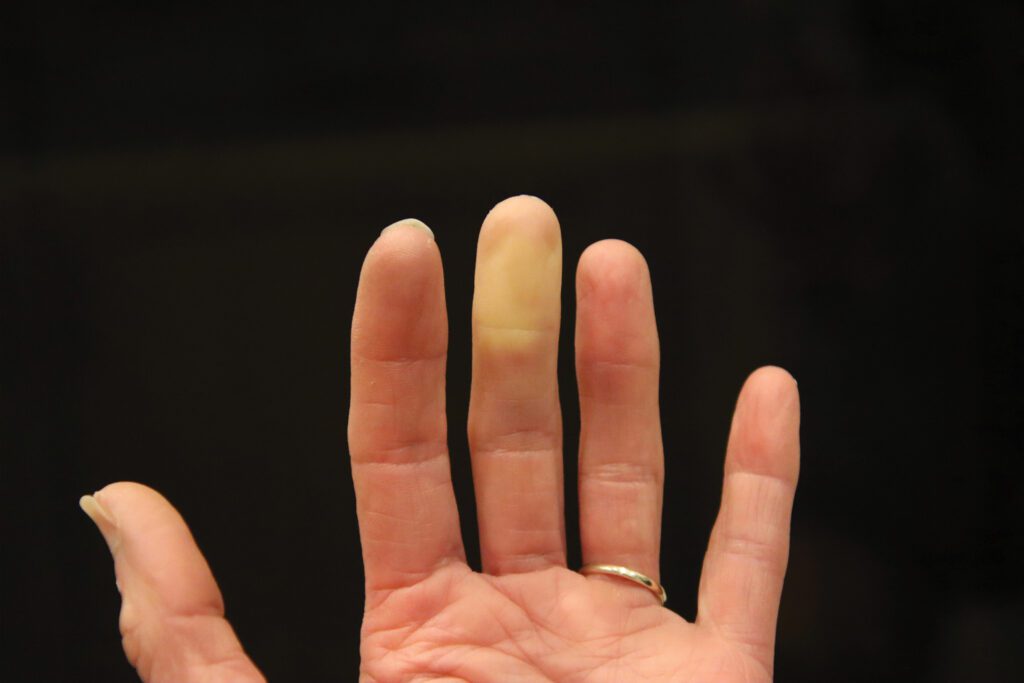
What is Raynaud’s?
Raynaud’s is a phenomenon in which the smaller arteries that supply blood to your skin narrow, limiting circulation in the extremities, causing them to turn white, red, or blue, and feel cold or numb. These vasospasms usually last just a few minutes, though severe cases might last as long as an hour or two. And while it seems obvious that these attacks typically occur in cold weather (or in the freezer section of the grocery store), stress can also cause an attack.
A reported 3-5% of the U.S. population have symptoms of Raynaud’s, and it’s overwhelmingly more common in women than in men. It can make wintertime extremely unpleasant, but only 1 in 5 seek treatment. The reasoning? Many people who have Raynaud’s symptoms assume it’s simply poor circulation, and leave it there.
However, the condition comes in two forms – one more serious than the other – so making a diagnosis is important.
Primary vs. Secondary Raynaud’s
Primary Raynaud’s is the most common form of Raynaud’s and is triggered by cold, stress, or smoking. In general, it tends to manifest between the ages of 15 and 30. It has no other obvious cause, but most people who develop it will have a close relative with it as well.
The secondary form, according to Dr. Indra K. Shah, a rheumatologist at the Parkridge Medical Center Campus, while less common, is potentially more serious. “Secondary Raynaud’s can occur in response to an underlying connective tissue disease like scleroderma (hardening and tightening of the skin and connective tissue) or lupus, or less commonly Sjogren’s syndrome (an immune system disorder) or rheumatoid arthritis. It can also be associated with obstructive diseases of the arteries, such as arteriosclerosis or Buerger’s disease (inflammation and/or clotting of blood vessels).” Certain medications, like beta blockers, can be responsible for secondary Raynaud’s too, as can nerve damage from occupational stress, like using jackhammers over a long period of time. Fortunately though, only a small number of those with Raynaud’s symptoms are diagnosed with the secondary form, which generally appears later in life, after 35.
“The diagnosis of Raynaud’s,” Dr. Shah explains, “is usually made based upon medical history, but further evaluation may require certain blood tests, and may include an arterial Doppler ultrasound and a nailfold vasculature study.“ In that study, a rheumatologist tests for secondary Raynaud’s by putting a drop of oil on the nail fold, the skin at the base of the fingernail. A microscopic view will indicate if there are enlarged or malformed capillaries, which could indicate a connective tissue disease. That would be followed by blood tests, the erythrocyte sedimentation rate and the antinuclear antibody test, which can help identify the underlying cause of Raynaud’s, and thus its treatment.
Managing Raynaud’s






Making smart lifestyle changes can lessen episodes of Raynaud’s. First, dressing warmly in winter months and paying attention to layers on extremities are the easiest ways to combat those painful frozen fingers and toes. And since the frozen-food aisle really will cause vasospasms, having gloves on while grocery shopping, even in the summer, is smart. Living in warmer climates is often suggested, though it’s not always feasible. At the least, take care to make slower transitions from a hot location to a cold one, like entering a well air-conditioned room from sweltering outdoors.
There are some medications that can help more severe cases, such as the family of calcium channel blockers, which dilate blood vessels, so blood circulates more easily. These are similar to high blood pressure medications though and won’t be appropriate for everyone.
One idea that has many adherents is windmilling the arms – done slowly so as to not damage the shoulder. Running warm water – not hot – over fingers or toes will restore color and feeling quickly without a strong burning sensation. Skin-to-skin contact warms fastest, so placing hands under armpits or massaging toes will help too. Exercise will even help cut down on spasms, since it increases circulation. However, those with secondary Raynaud’s should get advice from their doctor before exercising outdoors in the winter months.
If you’re a smoker, this is one more excellent reason to quit. Nicotine exposure lowers skin temperature by constricting blood vessels, and may lead to an attack.
For those whose attacks are triggered by stress, specialists recommend keeping a record of when you have attacks, and what the situations were that caused them. When you begin to recognize common factors that create stress and bring on spasms, find ways to avoid them. You can also practice some stress-reducing techniques like deep breathing, biofeedback (a process that uses electronic monitoring of an involuntary bodily function to train one to acquire voluntary control of that function), or other alternatives that work for you.
For severe cases, there are more aggressive treatment options. They include nerve surgery, where sympathetic nerves in hands and feet, which control the opening and narrowing of blood vessels, are removed through tiny incisions. Called a sympathectomy, it can reduce the number and duration of attacks. The second procedure involves injecting botulinum (Botox) into the sympathetic nerves of hands and feet, although it does wear off and must be repeated when attacks return.
If you have frequent or long-lasting spasms that are affecting your quality of life, it’s time to talk to your doctor. Dr. Shah shares, “When symptoms arise, see your doctor or rheumatologist for further evaluation. He or she can determine whether the problem is primary or secondary, whether additional studies are necessary, and if any treatment is required.”
For those with occasional attacks, managing Raynaud’s can be as easy as giving extra thought to your wardrobe. Luckily, living in Chattanooga means fairly short and mild bouts of cold weather, so you have controlled the biggest cause. Get regular exercise to keep your circulation going. Stock up on mittens and Alpaca socks, wear lots of layers, and remain calm. You should be feeling better already!


Dr. Indra K. Shah
Rheumatologist, Parkridge Medical Center Campus

